Is there hope for a treatment of kidney disease?
Chronic kidney disease (CKD) is a global health crisis that today affects a staggering one in 10 people worldwide, following explosive growth over the past several decades.
We’re clearly witnessing a silent epidemic of CKD, and improved pharmacotherapies are urgently needed. So where are we currently with developing therapeutics for kidney disease? What are the challenges – and is there reason for hope?
According to the WHO, kidney diseases are now the world’s 10th highest cause of death. Adding to this, even in its early stages CKD can also cause hypertension and significantly increase the risk of cardiovascular disease (the number one killer globally).
Diagnosis is relatively straightforward, but in most cases CKD does not cause any symptoms until it is well advanced and kidney or cardiovascular damage is irreversible.
If untreated or diagnosed late, CKD leads to obliteration of kidney function and end-stage renal disease.
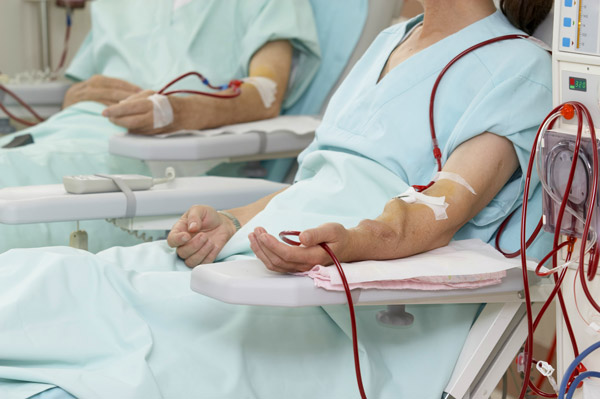
At this point, kidney failure patients have two options: going onto dialysis, where the blood is filtered through an external circuit, or transplantation.
 Important factors that may increase your risk of chronic kidney disease include:
Important factors that may increase your risk of chronic kidney disease include:
- Diabetes
- High blood pressure
- Cardiovascular disease
- Smoking
- Obesity
- Race/ethnicity
- Family history of kidney disease
- Abnormal kidney structure
- Age
Of these, the single most important risk factor and cause of chronic kidney disease worldwide is diabetes.
Approximately one-third of patients with type 2 diabetes develop diabetic kidney disease (DKD), making DKD the predominant cause of end-stage renal disease (ESRD). With this in mind, perhaps it’s not surprising that our current best hopes for a novel treatment seem to be stemming from the field of diabetic research.
A new hope
Recently, clinical trials designed to demonstrate cardiovascular safety of anti-diabetic medications have identified properties of some of the newer anti-diabetes drugs that go beyond pure anti-hyperglycemic action.
This includes, for example, the beneficial cardiovascular and renal effects of glucagon-like peptide-1 (GLP-1) agonists and sodium-glucose co-transporter-2 (SGLT2) inhibitors.
In the case of SGLT2 inhibitors, these orally available small molecules (which were developed to lower blood glucose levels by inhibiting glucose reabsorption at the site of the SGLT2 in the proximal tubule) have demonstrated strong effects on kidney endpoints such as albuminuria, GFR decline, kidney failure and death in DKD and lately in CKD patients.
Through these studies, it’s become apparent that SGLT2 inhibitors improve glomerular hemodynamic function, and are also thought to ameliorate other local and systemic mechanisms involved in the pathogenesis of CKD.
There are therefore great hopes around the possible potential of using SGLT2 inhibitors for treatment of CKD patients.
Lost in translation?
Despite emerging options with SGLT2 inhibitors on the horizon, there remains an unmet medical need for treatment of CKD today.
Unfortunately, modelling of kidney disease is incredibly challenging.
The kidney is one of the most complex organs in our body, and this complexity makes it both endlessly fascinating and almost impossible to mimic, particularly in in vitro systems.
Currently available in vivo models mimic several but not all aspects of the human condition. To get a better understanding of mechanisms leading to CKD and to develop new treatment options, translatable and stable rodent models that recapitulate features of human disease are essential.
While there are several well-established models for CKD – such as the Unilateral Ureter Obstruction (UUO) model, the 5/6 nephrectomy models, and the Adriamycin nephropathy model – the situation is different for DKD, especially when it comes to late-stage models.
For example, there’s a scarcity of models that combine hypofiltration and glomerulosclerosis in the context of diabetes and hypertension, and even less with demonstrated efficacy of known medications such as the discussed SGLT2 inhibitors.
As the race for new models continues, a selection of preclinical rodent models of CKD is currently based on existence of targeted pathways in a model. In combination with relevant endpoints, this gives novel therapeutics a chance of success.
We can also see that new technologies such as 3D bioprinting, organoids and organs-on-chips, as well as kidney slices, offer a great intermediate stage in the drug screening cascade.
They allow quick screening of putative therapeutics in a controlled environment. Based on initial characterisation of the novel treatment based on these technologies, therapeutics can be subsequently tested in the in vivo phase.
In the era of personalised medicine, we must acknowledge that we are not able to mimic every aspect of human disease in animal models. Although grouped into classes or categories, every person’s kidney illness is different.
However, by combining recent advances in technology with our most relevant animal models, we can provide the best possible evaluation of the disease mechanisms and prediction of the success of novel therapeutics.
So, while the kidney disease epidemic is vast and the translational challenges are significant, there is certainly reason for hope.
With new medications on the horizon, and new technologies to support our existing models, there is a real possibility that we could see effective therapeutics in the near future that can both save lives and improve them.
If you would like to speak to Sygnature about our significant experience in kidney disease drug development, contact us.
 Author: Author:Keld Fosgerau, PhD – CEO and Founder at Fosgerau Consult Keld is a drug development professional with 25 years of international experience leading companies, functions, departments and projects in virtual start-up, established biotech, CRO, and in large integrated pharmaceutical organizations from novel target discovery to early clinical development. |

