Chronic kidney disease (CKD) is a common and debilitating condition which affects an estimated 1 in 10 people worldwide. Individuals affected by CKD progressively lose kidney function as they are not diagnosed until the later stages of the disease due to the silent nature of this condition. Once diagnosed, control of blood pressure and inhibition of the renin angiotensin aldosterone system remains the cornerstone of the treatment of CKD. This slows disease progression but does not halt or reverse the condition. Consequently, biotech and large pharma are actively looking at improving their candidate screening cascades and testing platforms. This includes the use of precision cut kidney slices (PCKS).
The challenges for biotechs and big pharma developing treatments for CKD
#1 Lack of a translational bridge between in vitro, in vivo studies and the patient
Typically, in the classic R&D process before any lead candidate compounds are assessed in vivo, the properties of the drug and the mechanism of its possible mode of action are thoroughly evaluated using various vitro models. These in vitro assays often utilise one clonal cell type and thus fail to give any insight into the organ physiology and the greater translational response beyond the specific cellular cascade in question.
As the lead optimisation develops, animal models are increasingly used to evaluate the pathogenesis and underlying mechanisms of renal disease. Rodents (mice and rats) models are the most commonly used to study kidney injury and any potential therapeutic targets. Ethically the use of animals is carefully managed and utilised appropriately, aligning research with the 3r’S, so that only the most likely drug candidates are dosed in-vivo.
#2 Speed of screening and compound Use
Compounds in late lead optimisation once passing the in-vitro screening stage gate would typically enter into in-vivo model assessments. This requires scale up of test compounds, appropriate form pre-formulation support and the relatively slow throughput of in-vivo models.
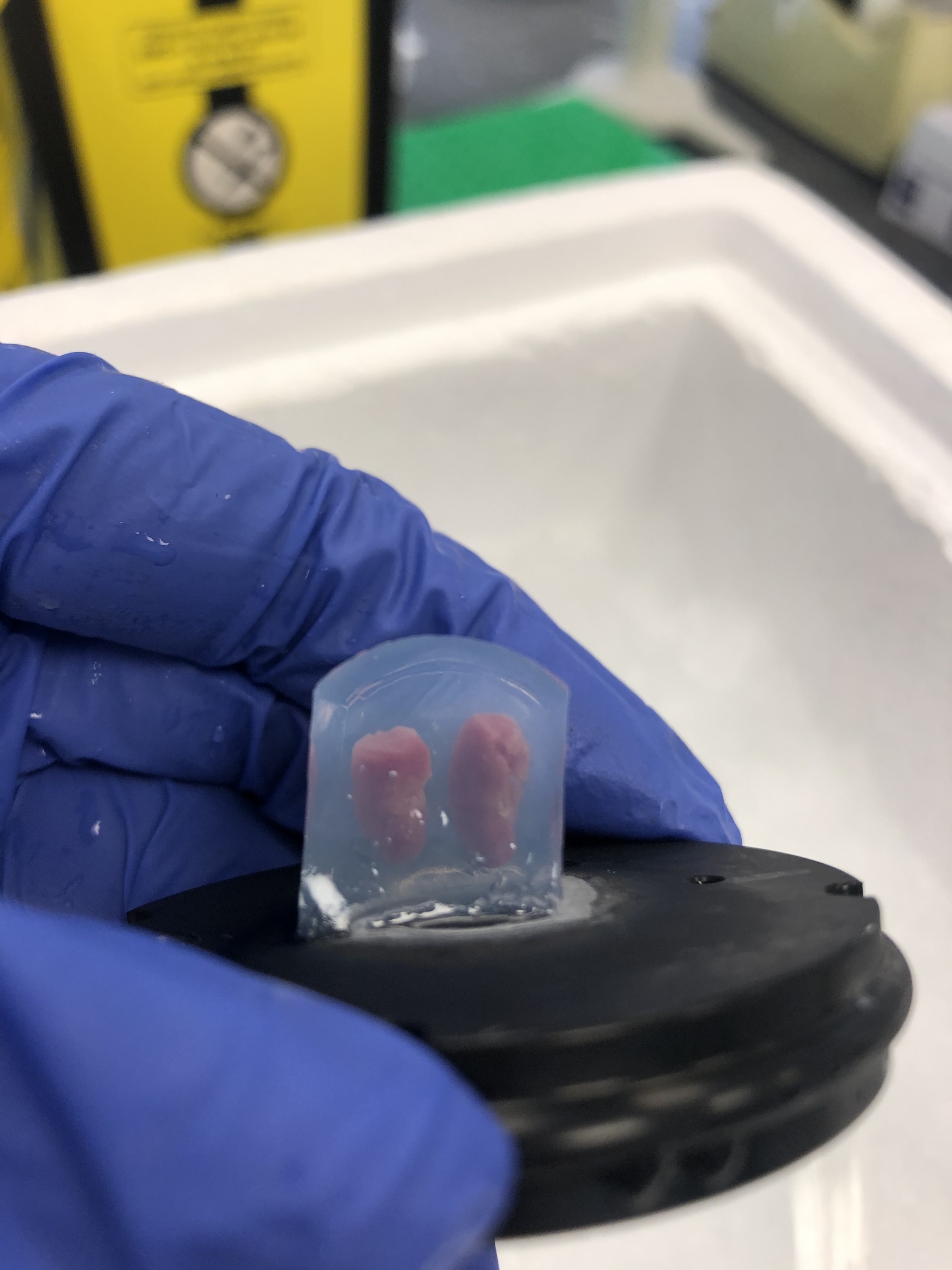
Precision cut kidney slices (PCKS) in the discovery cascade:
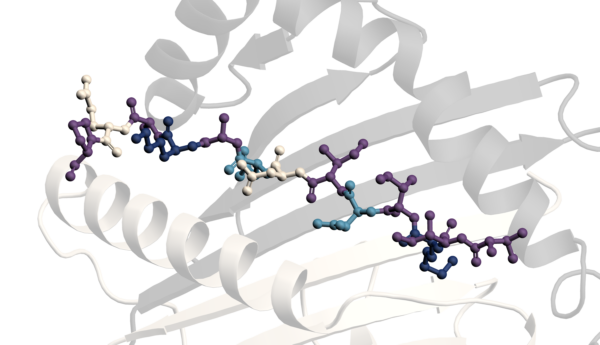
Precision cut tissue slices are three-dimensional (3D) tissue explants, usually derived from various human or animal organs, which can be cultured ex vivo for an extended period of time. All cell tissue (cortex, medulla) is present with intact inter-cellular and cell–matrix interactions.
These tissue slices, and in particular precision cut kidney slices (PCKS), represent a valid and robust platform to study the mechanism and efficacy of antifibrotic drug-candidates before moving into animal models.
Utilising precision cut kidney slices (PCKS) has several clear benefits in drug discovery:
- Higher throughput of lead candidates saving time and money around test material preparation and scale up etc.
- Faster selection of the nominated drug candidate
- Reduction in the number of animal models needed to be performed in candidate selection
- Consistency of test material reducing batch to batch variation
- Better translation into in-vivo and man utilising appropriate biomarkers
From one organ, researchers can obtain doses of the experimental units. And since they are more representative of the complex cell–cell and cell–matrix cross-talk than in vitro cultures, experimentation in slices offers a more reliable tool for drug candidate selection.
Further applications: exploring the benefits of human PCKS
The challenge with rodent tissue slices is that they are not human and theoretically do not fully translate into man. The use of kidney biopsy tissue from CKD patients as ex vivo disease models is a key addition or potentially in some cases an alternative to prolonged in vivo models. What’s more, using human PCKS allows ex vivo culturing of renal tissues in stasis for several days without the loss of the phenotype. This is becoming a popular and valid method in the pre-clinical screening cascade, addressing key questions around possible drug mechanism of action and its potential therapeutic properties in human diseased tissue. Direct comparison of data generated in human versus animal diseased tissues can also serve as a robust way of validating animal models that precede initial clinical trials.
Examples of potential biomarkers that can be used to bridge the translational gap from in-vitro, through ex-vivo tissue slices into man and in-vivo including rodents
- Increase in collagen production at mRNA and protein level, e.g. Collagen 1a
- Increase in fibronectin production (extracellular matrix deposition)
- Increase in alpha-smooth muscle actin (fibroblast transdifferentiation)
- Increase in inflammatory markers, cytokine release into media by PCKS and into plasma of kidney disease patients, e.g. IL6, TNF alpha
If you would like to hear more about the use and benefits of PCKS in Chronic Kidney Disease research contact Sygnature Discovery, today.
Additional reading material:
* The Lancet, volume 395, issue 10225, p709-733, February 29, 2020
Bigaeva, Emilia et al. “Transcriptomic characterization of culture-associated changes in murine and human precision-cut tissue slices.” Archives of toxicology vol. 93,12 (2019
Bigaeva, Emilia et al. “Predictive Value of Precision-Cut Kidney Slices as an Ex Vivo Screening Platform for Therapeutics in Human Renal Fibrosis.” Pharmaceutics vol. 12,5 459. 18 May. 2020
Stribos, Elisabeth G D et al. “Murine Precision-Cut Kidney Slices as an ex vivo Model to Evaluate the Role of Transforming Growth Factor-β1 Signaling in the Onset of Renal Fibrosis.” Frontiers in physiology vol. 8 1026. 12 Dec. 2017
Graaf, Inge Am de et al. “Precision-cut tissue slices as a tool to predict metabolism of novel drugs.” Expert opinion on drug metabolism & toxicology vol. 3,6 (2007): 879-98.
https://nc3rs.org.uk/who-we-are/3rs